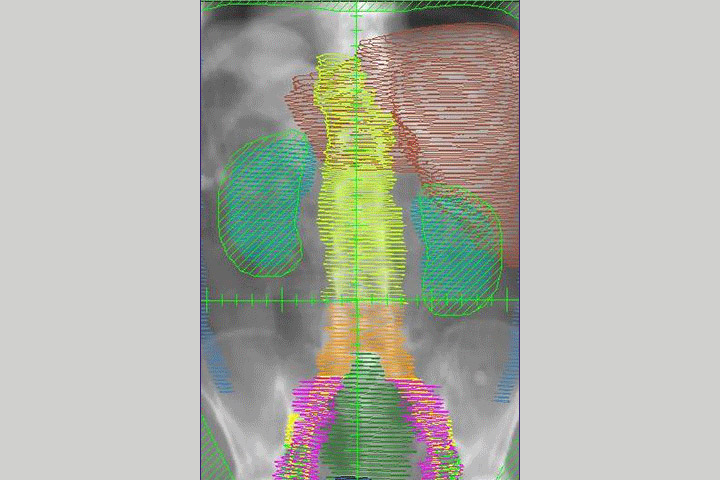
Stereotactic Body Radiation Therapy (SBRT) for Select Pancreatic Cancer Patients

As researchers search for ways to combat pancreatic cancer, one treatment gaining significant attention from the science community—and patients—is stereotactic body radiation therapy, or SBRT.
With traditional treatment, patients with early stage pancreatic tumors generally undergo surgery followed by chemotherapy, and sometimes radiotherapy as well. This conventional or standard radiation is delivered in relatively low doses, usually daily over the course of five to six weeks concurrently with chemotherapy.
An SBRT Primer
But with SBRT, higher doses of carefully targeted radiation are used to treat tumors, delivered in a few “fractionated” doses. “High doses of radiation are delivered over the course of only five days with limited toxicity,” explains radiation oncologist Joseph Herman, M.D., M.Sc., a leading researcher in the use of SBRT in pancreatic cancer.
Much of the credit for SBRT’s potential in treating pancreatic cancer has been due to technologic advances. “Basically what’s happened is that radiation technology has improved and now we have very sophisticated image guidance that pinpoints the exact three-dimensional location of a tumor,” he says. “That has allowed us to more precisely deliver radiation to tumors at much higher doses. These higher doses can lead to improved local control and possibly survival.”
Other improvements to the treatment include the control of a patient’s breathing motion since pancreatic tumors, like liver tumors, actually move during breathing. Doctors have developed ways to control for this phenomenon by tracking a patient’s breathing motion or directly managing it. “Essentially what we do is have a patient inhale deeply, hold that breath, and then we freeze the tumor in space and treat it,” says Herman, formerly professor and director of clinical research at MD Anderson Cancer Center, Houston, Texas (now at Northwell Health, New York). SBRT has also been aided through the use of fiducials—tiny gold markers—placed into the tumor that act as a kind of radiologic landmark, defining the target lesion’s position with millimeter precision, he adds.
Early Trials Answer Important Questions
In a multi-institution study published in the journal Cancer, Dr. Herman and colleagues treated 49 patients with locally advanced pancreatic cancer with SBRT. The patients received SBRT in five fractionated doses and chemotherapy with gemcitabine before and after the radiotherapy treatment. Four weeks after SBRT, all 22 patients who completed a quality of life questionnaire reported an eight point reduction in pain from a baseline measure of 25, and their quality of life stayed the same, which Herman says is encouraging.
In a second study, published in the Annals of Surgical Oncology, Herman and his colleagues analyzed information on patients with pancreatic cancer who received SBRT and chemotherapeutic drugs between 2010 and 2014. (Patients were treated at Johns Hopkins.) The study looked at acute and late toxicity of SBRT in locally advanced and borderline resectable pancreatic cancer.
Of 88 patients, eight experienced severe gastrointestinal side effects. Most of the patients who had side effects also had tumors that were invading into the intestines or stomach. For this reason, these patients should only get SBRT if the plan is to go to surgery following completion of SBRT. In this study, 19 patients with tumors previously considered inoperable (unresectable or locally advanced) were able to have surgery after SBRT. Several patients had a complete response at the time of surgery, meaning there was no tumor left behind.
To give people a surgical option is especially important since pancreatic tumors can often attach to and grow around blood vessels, making them difficult to remove, Herman says. “But after SBRT, the tumor actually changes to a form that can be more easily pried away from the vessel,” he adds, citing the current published data with SBRT over five days provides at least equivalent or better outcomes in terms of survival, with less toxicity, and better pathologic response rates than what is generally seen with standard treatment over five to six weeks. “In general, we don’t usually see this kind of response with standard radiation or chemotherapy alone,” he says.
Another factor to consider is that shorter treatment times with SBRT may provide other benefits such as allowing patients access to full-dose chemotherapy much more quickly than those undergoing standard radiation which, because of its longer schedule, potentially gives cancer more time to spread, he says.
Quality of life is also an important factor. “Most patients we treat with SBRT have tumors that can’t be removed by surgery and that means average survival is only about one year,” Herman says. “These patients generally have to go through about six weeks of standard chemotherapy and radiation. That can be difficult for patients and their families. But with SBRT it’s only about five days. That means patients spend a lot less time getting treatment and get to spend more time with family. I believe that’s incredibly important for everyone.”
Ongoing studies are testing combinations of SBRT with immunotherapy and researchers are also continuing to study the effectiveness of various radiation doses used in SBRT.
Looking To the Future
Based on current data, Herman is hopeful that more studies will lead to SBRT becoming a standard-of-care option for patients with locally advanced or unresectable and borderline resectable pancreatic cancer with blood vessel involvement. Patients with involvement of the stomach or duodenum are not good candidates for SBRT, unless they are surgical candidates.
“There’s a lot of work to be done, and I want to stress this is not a cure,” Herman says. “We absolutely need randomized trials and we need to figure out the optimal dose and fractionation that will sterilize tumors for patients,” For example, researchers must still determine how best to combine SBRT with targeted or immunotherapeutic agents. Personalizing treatment based on factors like genetics and the tumor microenvironment are also goals.
“Pancreatic cancer patients need more options, and we need the trials to determine what their best options may be,” Herman states. “SBRT provides another weapon in the battle against pancreas cancer.”