An Update on the Whipple Procedure

While inroads have been made in the medical treatment of pancreatic cancer, the best chance for a cure remains surgery
However, most studies show that only about one in five patients are diagnosed with pancreatic cancer that appears to be confined to the pancreas. For some of these patients, potentially curative surgery may be an option. The operation most often performed is called a pancreatoduodenectomy, or more colloquially a Whipple procedure, named after Dr. Allen Whipple, a Columbia University surgeon who was the first American to perform the operation in 1935. It is generally used to remove tumors that are confined to the head, or right portion, of the pancreas.
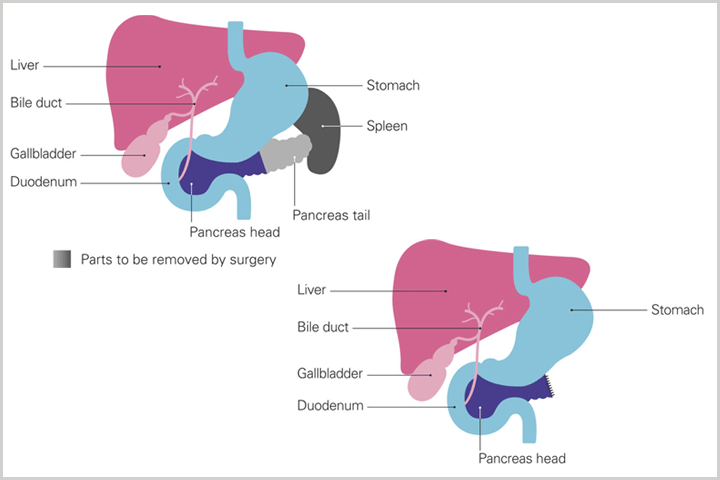
During this operation, the head of the pancreas and sometimes the body of the pancreas are removed. Part of the small intestine, part of the bile duct, the gallbladder, and lymph nodes near the pancreas are also removed. Sometimes part of the stomach is also removed. After removal of these structures, the remaining pancreas, bile duct, and the intestine are sutured back into the intestine to direct the gastrointestinal secretions back into the gut.
Although the procedure is complex, it has a long history of being performed successfully by surgeons who operate in high-volume centers, explains Dr. Michael Lieberman, Director of Surgical Oncology and Director of the Pancreas Center at NewYork-Presbyterian/Weill Cornell Medical Center. Surgeons there perform about 80 Whipple procedures every year, he says.
Indeed, the American Cancer Society recommends being treated by a surgeon who does many of these operations, and to have the surgery at a hospital where many of these operations are done. In general, people having this type of surgery do better when it’s done at a hospital that does at least 15 to 20 Whipple procedures per year, they say.
A Multidisciplinary Approach
The medical and surgical treatment of pancreatic cancer remains challenging. On the surgical front, doctors are investigating changes to improve outcomes and complications patients may face after a Whipple procedure.
Equally as important as technical expertise is the need for a multidisciplinary team approach to care. This team approach can more seamlessly provide adjuvant therapy, perioperative therapy, and nutrition expertise, for example, so that patients can thrive after surgery. “A Whipple can be a tough procedure for patients, but people can do very well when there are the right people providing ongoing care,” Lieberman says.
Although adjuvant therapy, such as chemotherapy, is often used to “mop up” any remaining cancer cells after surgical treatment, there is also a greater use of preoperative therapies, depending on the patient, to improve surgical outcomes.
These preoperative therapies, called neoadjuvant therapies, can include chemotherapy alone or chemotherapy and radiation therapy before surgery. This can be especially important for patients who are “borderline” resectable—whose tumors involve the nearby blood vessels. These patients may benefit from partial shrinkage of the tumor, which may allow a greater chance for complete removal of the cancer.
This neoadjuvant approach has been evaluated in several clinical trials, but it is still unclear whether neoadjuvant therapy improves survival rates, and more research needs to be done, Lieberman notes.
Minimally-Invasive Approaches Need More Study
Minimally invasive surgery, whether laparoscopic or robot-assisted, potentially offers a number of benefits to patients: less blood loss, quicker recoveries, and shorter hospital stays. Although these techniques are both being used more often in pancreatic cancer treatment, they represent only a small portion of the number of pancreatic cancer surgeries performed in the United States.
During a laparoscopic surgery, the surgeon inserts a thin, lighted tube with a camera on its tip through tiny abdominal incisions. In a robotic-assisted approach, the surgeon performs the procedure while seated at a console that includes a screen and hand, finger, and foot controls.
However, despite these technological advances, the traditional open Whipple procedure remains the mainstay of pancreatic cancer surgery, since more research needs to be done, explains Lieberman.
“The long and short of it is that most of the preliminary data shows that outcomes, including perioperative mortality, seem to be similar whether a procedure is performed traditionally, laparoscopically, or with robotic-assisted technology,” he says.
Some of the real benefits of minimally invasive techniques, such as smaller incisions, actually become a trade-off since these minimally-invasive approaches actually take longer to perform, Lieberman says. The average open Whipple procedure takes about four to six hours, while a laparoscopic operation may take up to six or eight hours. However, he expects that the length of time for the procedure may improve as more surgeons gain expertise in applying minimally invasive techniques to the Whipple procedure.
“I think there may be a real role for these approaches with distal pancreatectomy,” says Lieberman. During this procedure, surgeons remove the spleen and only the tail of the pancreas or the tail and a portion of the body of the pancreas. This procedure is generally used to treat pancreatic neuroendocrine tumors, rather than the more common exocrine pancreatic cancers.
As a surgeon treating pancreatic cancer patients, Lieberman is hopeful about current research improving the outcome for pancreatic cancer patients.
“We are learning more about pancreatic cancer than ever before, and I think we are entering a time in which fairly soon we are going to see some definite improvements in the earlier detection of the disease, a time in which potentially curative surgery may be an option for more patients,” he says.