Understanding Distal Pancreatectomy
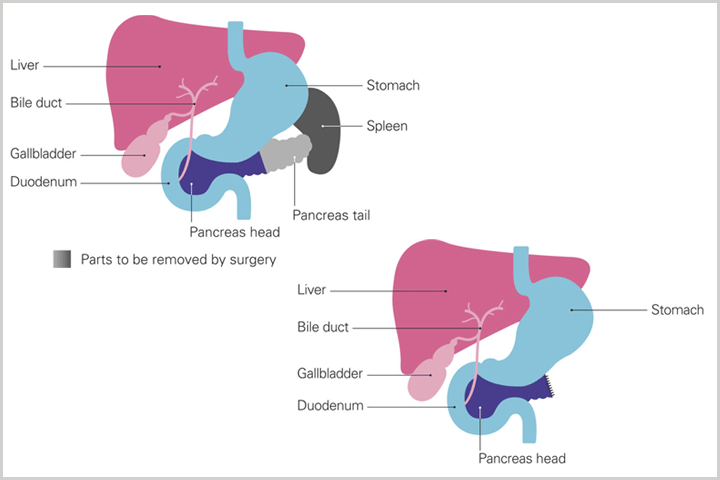
If your cancer is operable, the type of surgery you get will be based on the location of your tumor.
When people think about pancreas surgery, the word Whipple comes to mind. The famously complicated and demanding surgery, officially called a pancreatoduodenectomy, takes anywhere from four to twelve hours to complete and involves the moving around of several organs.
Fewer people are familiar with its less famous cousin, the distal pancreatectomy. What’s the difference, and how do doctors decide which one is appropriate for each patient?
To put it simply, the Whipple is performed on the head of the pancreas, while the distal pancreatectomy is for tumors located in the body and/or tail (thin end) of the pancreas.
Even though a distal pancreatectomy is less complicated than the Whipple procedure and considered minimally invasive, with faster recovery time and less severe side effects, it is still major surgery.
What to Expect during a Distal Pancreatectomy
Patients are put to sleep for the procedure, which generally lasts around four hours. During the procedure, the abdomen is filled with gas to give the surgeon greater visibility of the pancreas and abdominal cavity. Two sets of tubes are inserted through the patient’s nose, into the stomach, to help prevent nausea/vomiting and to help fluids drain out during the surgery and during recovery.
There are usually three incisions in the abdominal wall: one for a camera, one for surgical equipment, and one for the surgeon’s hand. The remaining part of the pancreas will be closed with sutures (stitches) or staples.
The Spleen: Remove or Not?
The tail of the pancreas is nestled within the spleen, and the blood vessels that feed the spleen run right behind the pancreas. Often, the fist-sized immune organ is also removed during a distal pancreatectomy.
How do doctors decide whether to save the spleen or remove it? It depends on the type of tumor you have.
If it’s a more benign or precancerous tumor, surgeons may do a spleen-preserving procedure, where they just remove the tail of the pancreas. If the tumor is cancerous or suspected to be cancerous, they are likely to remove the spleen along with the pancreas.
There are a couple of reasons for this. First of all, there are a lot of lymph nodes surrounding the tail of the pancreas and spleen, and removing the spleen as well as the tail of the pancreas reduces the risk of the cancer spreading to the lymph nodes; it also increases the chances of capturing any spread that has already started.
Secondly, there may be a need to remove the artery and vein that feed the spleen in order to get to the tumor.
Although the spleen is extremely important in children and adolescents because of its immune function in filtering blood and controlling infection-fighting white blood cells, it has less importance as we get older.
At some hospitals, if the spleen is removed patients are given a trivalent (three-part) vaccine to protect against the biggest infections they might face: pneumococcal pneumonia, H. influenzae (bacterial version of flu), and meningitis.
Other patients take long-term antibiotics after surgery, and all patients should inform their physicians that they’ve had their spleen removed, in case they require a different antibiotic treatment for other infections.
Possible Side Effects
One of the most common complications after surgery is the leakage of digestive juices from the pancreas, estimated to occur in 20-30 percent of patients.
To combat the problem, doctors can insert a drain that comes out of the patient’s left side and empties into a small container. It is usually removed by the time the patient leaves the hospital.
Delayed gastric emptying also happens in 15-20 percent of patients. The stomach, which is located near the surgical site, empties slowly, causing patients to feel full more quickly or to have upper abdominal discomfort that prevents them from wanting to eat.
A consultation with an oncology dietitian can help alleviate this.
About 60 percent of the body’s insulin production is located in the tail of the pancreas, so people with diabetes could face an altered need for pills or insulin to control their condition. Others may need supplementary insulin immediately after the surgery but return to normal later. And yet others with healthy blood sugar levels may experience no difference.
The same goes for the need for supplementary digestive enzymes. If a patient’s pancreas doesn’t make enough digestive enzymes after surgery, they may have diarrhea. If this happens, they can take enzyme pills when they eat. Luckily, most digestive juices are made in the head of the pancreas, so there will likely be enough of the pancreas remaining to prevent this problem.
The majority of patients tolerate the surgery quite well. The hospital stay should be approximately five days, and most patients will go home either on a regular diet or a low-fat diet.






