Reducing Pancreatic Cancer Disparities Through the NCI Community Oncology Research Program (NCORP)
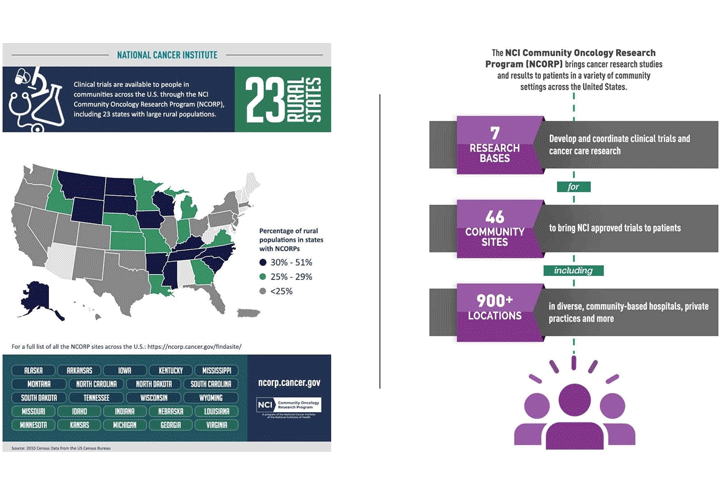
Whether you live in the heart of a major city or in a remote rural community, Dr. Worta McCaskill-Stevens is determined that you will have access to quality cancer care.
As Director of the NCI Community Oncology Research Program (NCORP), the medical oncologist has reason to be hopeful. The national network of investigators, cancer care providers, academic institutions, and other organizations has successfully enrolled thousands of patients from diverse communities across the United States in multi-site clinical trials since its formation in 2014.
This is important because, according to a 2018 study in the Journal of the American Medical Association (JAMA), the differences in survival rates between rural and urban patients are significantly reduced when patients are enrolled in a cancer clinical trial. “In trials, patients are uniformly assessed, treated, and followed under a strict, guideline-driven protocol,” says Joseph Unger, Ph.D., a health services researcher and biostatistician at the Fred Hutchinson Cancer Research Center, Seattle, Washington, who led the NCORP-funded study. “This suggests that giving people with cancer access to uniform treatment strategies could help resolve the disparities in outcomes that we see between rural and urban patients.”
A Corps of Cancer Care Delivery
Cancer clinical research has traditionally been conducted at academic medical centers, but most cancer care actually takes place in the community setting. Being able to join research studies in a person’s own community allows the person to stay close to family, friends, support systems, and their local physicians and health organizations, explains McCaskill-Stevens.
“Expanding clinical research beyond the academic environment allows access to a larger and more diverse patient population in a variety of ‘real world’ healthcare settings,” she adds. “This can accelerate accrual to clinical trials, enable feasibility testing of promising new interventions, and increase the generalizability of study findings.” Engaging community oncologists in collaborative research can also facilitate the uptake of effective, evidence-based practices into routine care, McCaskill-Stevens notes.
NCORP includes seven research bases, which serve as hubs to design and conduct multi-center clinical trials and cancer care delivery research studies, and 46 community sites to accrue study participants and engage community partners. At NCORP’s most recent annual meeting, in September 2018, McCaskill-Stevens reported that the growing program now has 960 component and subcomponent sites.
NCI Director Norman (Ned) Sharpless, M.D., (at the time of this story) appreciates the work NCORP has done to bring clinical trials and care to communities across the country, and has committed to an increase in NCORP funding. “NCORP is a way whereby we can provide great care and clinical research to patients we wouldn’t be able to reach otherwise,” Sharpless said at the meeting.
Equality Instead of Cancer Disparities
One of the core missions of NCORP is to address and reduce cancer disparities—cancer-related problems that disproportionately affect racial/ethnic minorities and underserved populations. To help accomplish this, the program has 12 specially designated minority/underserved community sites in areas with patient populations comprising at least 30 percent racial/ethnic minorities or rural residents.
One of these sites is the John H. Stroger, Jr. Hospital of Cook County. Located in the Illinois Medical District on Chicago’s Near West Side, the hospital is the largest component of the safety net for healthcare in Chicago and suburban Cook County. Its participation in the network has been a resounding success, recruiting more than 1,715 patients to clinical trials, and publishing several studies in peer-reviewed academic journals and conferences.
“Our mission is to address the shortage of accessible cancer healthcare resources for Chicago’s poor and minority families,” says site director Thomas E. Lad, M.D. “The clinical trial menu that is chosen for activation is designed with a view toward the minority population and type of cancers seen at our hospital.”
Education and outreach are also important activities at the site, as well as the program as a whole. In addition to clinical studies, NCORP’s social scientists also examine how financing systems, organizational structures/processes, health technologies, and healthcare provider and individual behaviors affect cancer outcomes, access to and quality of care, cancer care costs, and the health and well-being of cancer patients and survivors.
Ann Geiger, Ph.D., NCORP’s lead scientist for its Healthcare Delivery Research program, explains that understanding and addressing health disparities will continue to be a focus over the next couple of years. Populations of specific interest include adolescents and young adults, the elderly, racial and ethnic minorities, sexual and gender minorities, and rural residents.
As she reported at the group’s annual meeting, pancreatic cancer will be a particular focus in 2019. In order to investigate the link between new-onset diabetes and pancreatic cancer, NCORP is helping to enroll 4,000 patients to the New Onset Diabetes Cohort study. The goals of the study—which is also backed by the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) and the Pancreatic Cancer Detection Consortium (PCDC)—are to identify and follow a large cohort; develop a biorepository; clinically validate promising biomarkers of pancreatic ductal adenocarcinoma (PDAC); and develop an early detection protocol for sporadic PDAC.