The Stroma Presents Challenges and Treatment Opportunities
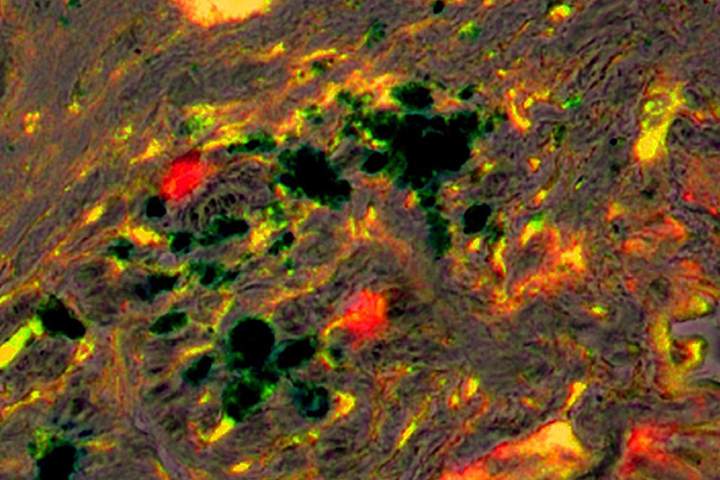
Hongyu Zhou, Lily Yang National Cancer InstituteEmory University
Pancreatic cancer is a tough-to-treat malignancy.
Fortunately, there have been some significant improvements in therapies that are benefiting more patients. One of the continuing challenges facing researchers is the stroma, and the role it plays in making pancreatic cancer so resistant to treatment.
What Is the Stroma?
In terms of basic biology, organs and glands all have a stroma, which is easiest to think of as a kind of framework made up of connective tissue. The iris of your eye has a stroma; so do a woman’s ovaries, as do other body parts, including the pancreas. The cells of the stroma have a job to do, which is to provide support, structure, and anchoring for the organs that exist inside of us. These stromal cells reduce stress on the organ by helping it function where and when it has to within the body.
That means the stroma is a necessary component in human biology and it’s this matrix of cells that allow an organ to simply stay in place, explains Dr. Elizabeth Jaffee, Deputy Director, The Sidney Kimmel Comprehensive Cancer Center at Johns Hopkins and an international leader in developing immune-based therapies for pancreatic cancer. She also leads the Stand Up To Cancer-Lustgarten Foundation Dream Team: Transforming Pancreatic Cancer to a Treatable Disease.
But with pancreatic cancer, the stroma, which normally quietly goes about its job of supporting an organ, takes on a much more pivotal role. “Pancreatic cancer is one of those cancers that seems to depend quite significantly on the stroma, and it’s a very complex relationship,” Jaffee says. Add into the mix that the stroma of a pancreatic cancer tumor is also very dense or “desmoplastic” as scientists often refer to it, which is one reason why drugs traditionally used to treat pancreatic cancer have such a tough time reaching their target.
Shining a Light on the Stroma
But today, scientists are looking at the stroma in a new light when it comes to pancreatic cancer. “We are continually learning more about the stroma and pancreatic cancer, and we’ve transitioned through a lot of different phases,” Jaffee says. At one time, for example, scientists thought the stroma had only one role, and that was as a “bad actor,” making it difficult for chemotherapy to reach the pancreatic tumor. But scientists also learned the stroma may actually have a kind of protective effect in terms of pancreatic cancer by compromising the ability of the cancer to spread.
“What we learned is that you don’t want to eliminate the stroma completely or too quickly, because those tumors can become even more aggressive,” Jaffee says, adding that this may be one of the reasons certain drugs that have been tested in that environment have failed. “We used to think that treating cancer was all about attacking and eradicating the cancer cells. But we’ve come to realize that we’re not only treating and attacking the cancer cell, but the surrounding stroma, the microenvironment, as well,” she adds.
Stroma Biology Plays a Role
Researchers are also learning more about the basic biology of the stroma. Just recently, researchers found two varieties of a specific cell type called fibroblasts. These fibroblasts help create the stroma. The hope is that selectively targeting these fibroblast subtypes will boost the ability of drugs to treat pancreatic cancer more effectively.
Another area of research focuses on the interaction between the stroma and surrounding structures, such as the epithelial component, and how they talk to, or signal, each other. There is also ongoing research looking at how pancreatic cancer takes advantage of the stroma to secure nutrition, such as proteins and other nutrients, which help it grow. The goal of the research would be to find therapeutic targets for intervention.
Researchers are also investigating agents that disrupt the stroma in a targeted way. For example, one agent is called PEGPH20. It specifically targets hyaluronic acid (HA), which is very important to the composition of the stroma. The hope is that disrupting and breaking down HA may allow chemotherapy to reach its target and kill pancreatic cancer cells.
Immunotherapy and the Stroma
Scientists are also looking to shed new light on how the immune system is suppressed within the stroma, or what researchers often refer to as the tumor microenvironment. “Pancreatic cancer is not naturally immune responsive and so what we want to do is lift this suppression so that the antitumor immune responses can be improved,” says Jaffee.
Tumor immunologists have long observed that, within the cancer stroma, immune cells are somehow suppressed, probably by nontumor cellular components. So finding the specific cells within the complex mixture of the cancer stroma that prevents immune killing is an important step in improving immunological therapies for the disease.
For example, Jaffee’s team is looking for ways to dismantle the stroma by targeting a specific checkpoint called CXCR4. “If we can alter the amount of stroma with a compound, we can combine it with a T cell-inducing approach such as a vaccine to see if the T cells can get at the tumor more effectively,” she says, adding that pre-clinical trials look promising.
The research is moving forward, and Jaffee is hopeful about the future. “I’ve seen tremendous changes in the way we approach pancreatic cancer just in the last several years,” she says. “We are learning more about the microenvironment all the time, and that is vital to improving treatment. I’m hopeful, but I’m also confident that we are going to get the answers we need.”
In a video, Dr. David Tuveson explains the structure of pancreatic tumors, including the stroma.